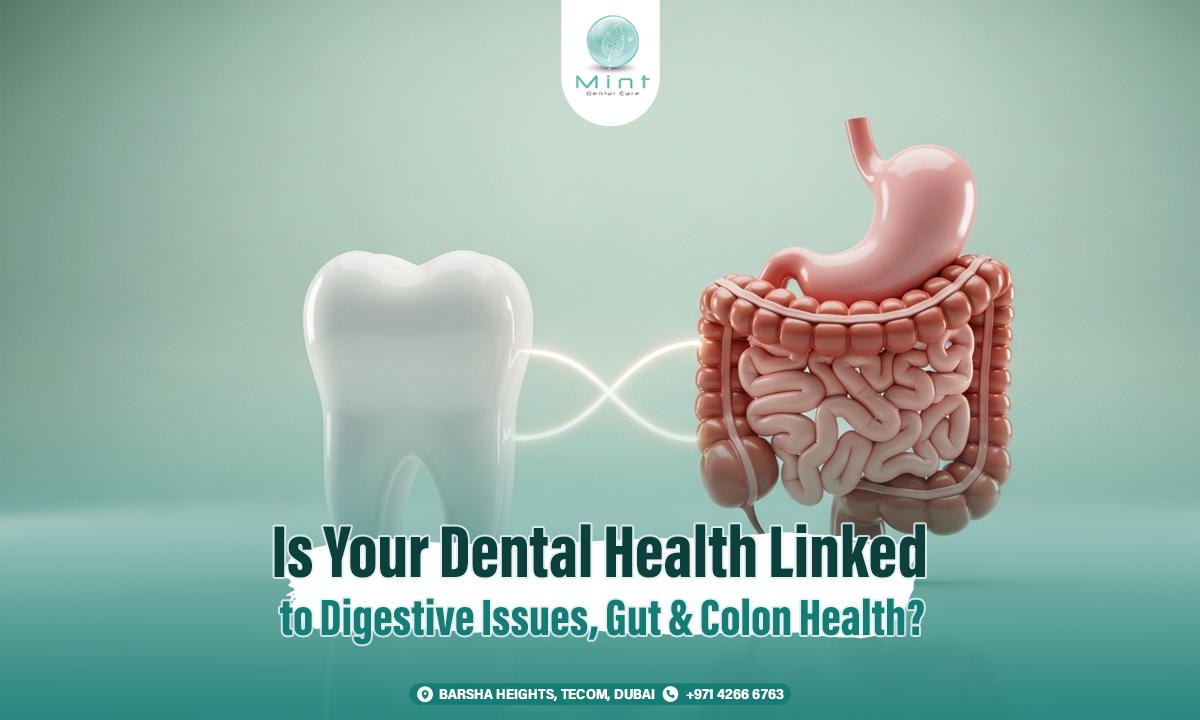
Many people think of the mouth and the digestive system as two separate parts of the body. In reality, they are closely connected. Your mouth is the beginning of the digestive tract, and changes in your teeth, gums, tongue, saliva, and oral tissues can sometimes reflect what is happening deeper in the body. This is why more patients today are asking an important question: is your dental health linked to digestive issues, gut and colon health?
At Mint Dental Care, we believe modern dentistry should look beyond the teeth alone. Oral health is often influenced by hydration, nutrition, inflammation, medications, immune balance, and everyday habits. In some cases, digestive issues such as acid reflux, chronic dry mouth, nutrient absorption problems, or inflammatory bowel conditions may affect your oral health in noticeable ways. In other cases, ongoing gum disease and oral bacteria may be part of a wider conversation about whole-body health and the so-called oral-gut axis. Research continues to explore these links, especially around oral inflammation, systemic health, and the movement of microbes between the mouth and gastrointestinal tract.
This does not mean every stomach problem will damage your teeth, or that every dental issue points to a gut condition. But it does mean the connection is real enough to deserve attention. If you are searching for clear advice from a trusted dental clinic in Dubai, this guide explains how oral health and gut health may be connected, which digestive conditions can affect your teeth and gums, and when it is time to seek professional help.
Understanding the Oral-Gut Connection
The mouth is the first stop in the digestive system. Food enters through the mouth, where chewing begins and saliva starts the early stages of digestion. But the connection goes beyond digestion itself. The mouth has its own microbiome, made up of bacteria and other microorganisms. The gut has its own microbiome too. Scientists now study how these two environments may influence each other, especially when inflammation or bacterial imbalance is present.
Saliva plays an important role in this connection. It helps protect the teeth, lubricate the mouth, support swallowing, and maintain a healthier pH balance. It also helps control bacteria. When saliva is reduced, oral tissues become more vulnerable to tooth decay, gum irritation, fungal infection, and bad breath. Saliva also supports swallowing and digestion, which is one reason dry mouth can affect both comfort and oral health.
From a clinical point of view, dentists often notice signs in the mouth that may be linked to digestive issues. These signs do not replace a medical diagnosis, but they can be useful clues. That is why understanding digestive issues and oral health matters so much.
Can Digestive Issues Show Up in the Mouth?
Yes, in many cases they can. Some digestive problems affect the mouth directly, while others create changes through acid exposure, inflammation, nutrient deficiencies, medication side effects, or dehydration. The result may appear as enamel erosion, mouth ulcers, gum irritation, dry mouth, sensitivity, burning sensations, or unpleasant breath.
At Mint Dental Care, we often remind patients that the mouth can be an early warning system. Persistent symptoms such as unexplained sensitivity, oral sores, frequent bad breath, sour taste, gum inflammation, or rapid enamel wear should never be ignored. While not every symptom points to a gut or colon problem, some deserve a closer look.
Acid Reflux and Your Teeth
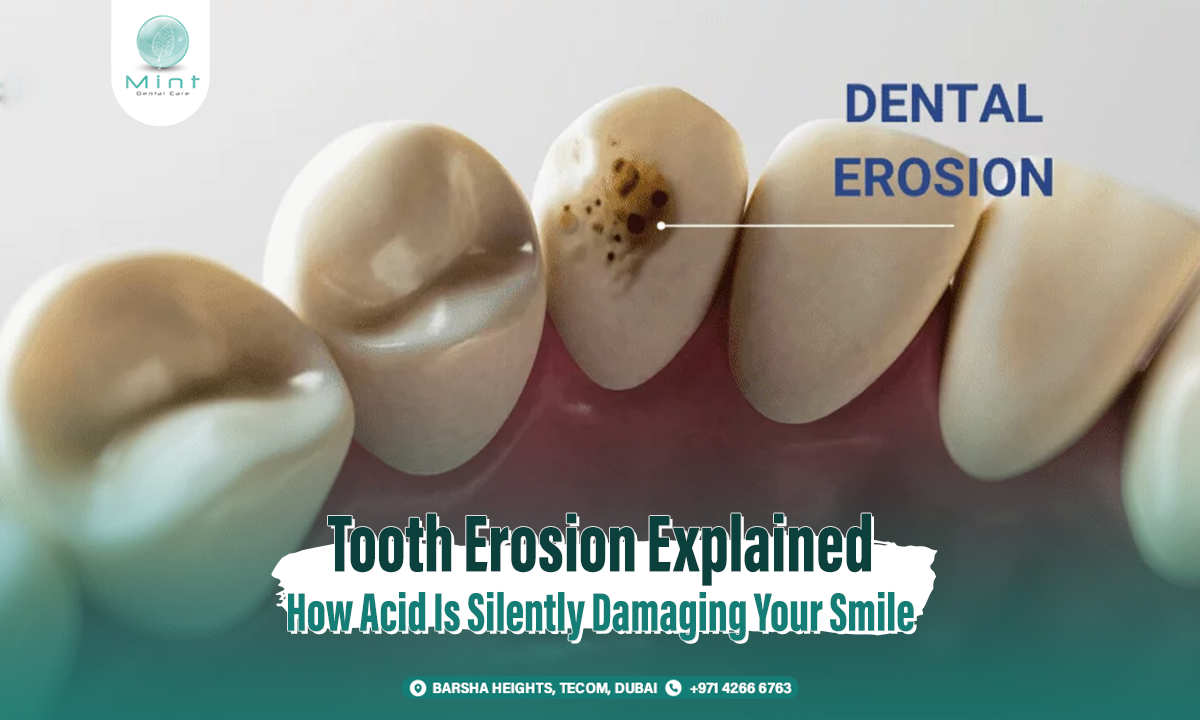
One of the clearest examples of the connection between digestive issues and oral health is acid reflux, also known as GERD when it becomes chronic. In reflux, stomach acid travels upward into the esophagus and sometimes reaches the mouth. Because stomach acid is highly acidic, repeated exposure can gradually wear away tooth enamel.
This erosion often affects the inner surfaces of the teeth first, especially the upper teeth, though the exact pattern can vary. Over time, patients may notice increased sensitivity, smooth or thinning enamel, discoloration, or teeth that seem more fragile than before. Some dentists are among the first healthcare professionals to suspect GERD because they see patterns of enamel erosion that do not match ordinary brushing wear alone. Reviews of the evidence have found that tooth erosion is a recognized oral manifestation of GERD, and MedlinePlus notes that reflux can cause acid or food to reach the back of the mouth.
This is important for patients in Dubai who may already consume acidic drinks, coffee, citrus, or carbonated beverages. When reflux is added to the picture, enamel may weaken faster. The result is not only cosmetic. Once enamel is lost, teeth may become more sensitive and more vulnerable to wear and decay.
Why Dry Mouth Matters for Both Oral and Digestive Comfort
Dry mouth is another major factor in the relationship between oral health and gut health. Some digestive conditions, medications, dehydration, or reduced saliva flow can leave the mouth feeling dry, sticky, or uncomfortable. When saliva decreases, the mouth loses one of its main protective tools.
Without enough saliva, food particles and bacteria are not cleared as effectively. Acids stay active longer, and the risk of tooth decay rises. The mouth may also feel sore, the tongue may burn, and swallowing may become less comfortable. MedlinePlus notes that dry mouth raises the risk of tooth decay, and the ADA explains that reduced saliva can contribute to dental caries, mucositis, fungal infections, and periodontal disease.
Patients with ongoing digestive symptoms sometimes focus entirely on abdominal discomfort while overlooking the dryness in their mouth. But that dryness may be quietly affecting their gums, tongue, teeth, and breath. At Mint Dental Care, we look carefully at saliva-related changes because dry mouth can turn a small dental risk into a bigger one over time.
Inflammatory Bowel Disease, Gut Inflammation, and Oral Signs
When people ask about gut and colon health signs in the mouth, one of the most relevant areas is inflammatory bowel disease, or IBD. This includes Crohn’s disease and ulcerative colitis. These are chronic inflammatory conditions that affect the digestive tract, but they may also have oral manifestations.
Scientific reviews describe several oral findings linked to IBD, including aphthous-type ulcers, mucogingivitis, swelling, cobblestoning, mucosal tags, and other inflammatory changes. Some studies also suggest a relationship between IBD and periodontal disease through shared inflammatory pathways and the oral-gut axis, although this remains an area of ongoing research rather than a simple one-way cause-and-effect story.
This means your dentist may sometimes notice recurring ulcers, inflamed tissues, or unusual oral lesions in a patient who also has digestive symptoms or a known bowel condition. That does not mean a dentist diagnoses colon disease from the mouth alone. But it does mean oral signs can be part of the bigger clinical picture.
Can Colon Health Affect Gums and Teeth?
The phrase colon health and oral health has become more common because people are increasingly aware that inflammation is not always isolated to one body system. In conditions involving the bowel, inflammation, nutrient disruption, medication use, and immune changes can all influence oral tissues.
For example, patients with inflammatory bowel conditions may be more likely to experience mouth ulcers, gum irritation, and soft tissue discomfort. Some may also struggle with oral hygiene when symptoms flare, simply because they are tired, dehydrated, or focused on managing gastrointestinal symptoms first. Emerging reviews of digestive disease and oral health also discuss how some patients with IBD may have higher rates of periodontal disease and tooth decay than healthy controls, though researchers continue to investigate the exact mechanisms and whether the relationship is direct, shared, or bidirectional.
The key message is not fear. It is awareness. If you already live with a bowel condition, your mouth deserves extra attention, especially when symptoms change.
Nutrient Absorption Problems and Oral Health
Digestive health does not only affect the mouth through acid and inflammation. It can also affect oral tissues through nutrition. When the body struggles to absorb nutrients properly, the mouth may be one of the first places to show signs of deficiency. Iron, folate, vitamin B12, and other nutritional deficiencies can contribute to mouth soreness, ulcers, burning sensations, and changes in the tongue or soft tissues.
This is particularly relevant in patients with long-term digestive disorders, restricted diets, chronic inflammation, or medication-related changes. While these signs are not specific to gut disease alone, they are part of the reason dentists pay attention to the whole health picture rather than isolated tooth symptoms.
At Mint Dental Care, we always encourage patients with recurring mouth ulcers, unexplained soreness, or soft tissue changes to seek a proper dental evaluation and, when needed, medical follow-up as well.
Vomiting, Nausea, and Enamel Damage
Another way digestive problems may affect the teeth is through frequent vomiting or regurgitation. Repeated exposure to stomach acid can soften enamel and increase erosion, especially if teeth are brushed immediately after the acid exposure. Enamel that has already been weakened becomes more likely to wear down, stain, chip, or feel sensitive.
This is one reason why patients with reflux, chronic nausea, or other acid-related digestive issues should not ignore dental sensitivity. What looks like a simple sensitivity problem may actually be acid damage over time.
Can Poor Oral Health Affect the Gut Too?
This is where the discussion becomes especially interesting. The traditional view is that digestive issues affect the mouth. But growing research suggests the relationship may go both ways. Scientists are studying whether harmful oral bacteria and chronic gum inflammation may influence wider systemic inflammation and potentially contribute to changes beyond the mouth, including in the gastrointestinal system.
Research on the oral-gut axis suggests that oral microbes can reach the gut and may play a role in broader disease processes under certain conditions. At the same time, reputable organizations such as the ADA and Mayo Clinic emphasize that oral health is closely linked to overall health, while also making it clear that many of these relationships are still being actively studied. In other words, there is enough evidence to take the connection seriously, but not enough to oversimplify it into a direct rule that bad teeth automatically cause colon disease.
For patients, the practical lesson is simple. Good oral hygiene supports more than just a nice smile. It helps reduce plaque, bacterial load, and chronic gum inflammation, all of which are worth managing for both oral and general health.
Signs in the Mouth That May Be Worth Investigating
There are several oral symptoms that may justify a closer look, especially if they occur alongside digestive complaints. These include ongoing dry mouth, recurring ulcers, sour taste, bad breath that does not improve, frequent tooth sensitivity, visible enamel wear, burning mouth sensations, red or swollen gums, and discomfort when swallowing or chewing.
None of these signs alone prove a gut or colon condition. But if they are persistent, recurring, or combined with symptoms such as reflux, bloating, abdominal pain, bowel changes, or chronic inflammation, they should not be ignored.
As a patient-centered dentist in Dubai, we believe in paying attention to patterns. Often, it is the pattern of symptoms rather than one single sign that gives the most useful information.
How Mint Dental Care Helps Patients Protect Their Oral Health
At Mint Dental Care, we take a comprehensive approach to prevention and diagnosis. If a patient presents with signs of acid wear, gum inflammation, oral soreness, dry mouth, or unexplained sensitivity, we assess not only the teeth but also possible lifestyle and health factors that may be contributing.
Our clinic offers routine dental checkups, professional cleaning, cosmetic dentistry, restorative care, gum evaluation, children’s dentistry, orthodontic treatment, and advanced diagnostics in a calm and modern setting. This matters because early dental findings can sometimes help patients understand a broader health issue before the damage becomes more severe.
For example, identifying reflux-related enamel erosion early may help protect the teeth before significant tissue is lost. Recognizing dry mouth early may help reduce the risk of future cavities. Noticing recurrent ulcers or gum changes may lead to timely medical conversations that support the patient’s general well-being.
What You Can Do to Protect Your Teeth if You Have Digestive Issues
If you live with reflux, chronic digestive symptoms, IBD, dry mouth, or frequent nausea, there are several smart ways to protect your smile. Stay well hydrated, avoid constant sipping of acidic drinks, and maintain consistent brushing and flossing habits. If reflux is part of the problem, speak to both your physician and your dentist so the teeth and the underlying condition are managed together.
Patients with dry mouth may benefit from more frequent hydration, saliva-supportive habits, and dentist-recommended products. Those with sensitivity or enamel erosion may need fluoride-based support and regular monitoring. Most importantly, do not wait for pain before booking a checkup. Digestive-related dental damage can begin quietly.
When Should You See a Dentist?
You should schedule a dental visit if you notice persistent bad breath, unexplained sensitivity, thinning enamel, recurring mouth ulcers, gum irritation, dry mouth, or a sour taste in the mouth that keeps returning. These may be signs that your oral environment is under stress.
You should also seek medical evaluation if oral symptoms are paired with digestive complaints such as chronic reflux, swallowing difficulties, abdominal discomfort, bowel changes, or signs of nutrient deficiency. Dentistry and medicine often work best together in these cases.
Final Thoughts: Is Your Dental Health Linked to Digestive Issues, Gut and Colon Health?
The answer is yes, in many cases there is a meaningful connection. The mouth and digestive system are closely linked through saliva, acid exposure, inflammation, nutrition, medication effects, and the oral-gut microbiome. Conditions such as GERD, dry mouth, inflammatory bowel disease, and nutrient absorption problems may all leave signs in the mouth. Research also suggests that oral bacteria and chronic gum inflammation may be part of a broader conversation about whole-body health and the gut, even though many details are still being studied.
The most important takeaway is this: your mouth should never be treated as separate from the rest of your health. If something feels off in your teeth, gums, tongue, or breath, it deserves attention. Sometimes protecting your smile also means understanding what may be happening deeper in the body.
Book Your Consultation at Mint Dental Care
At Mint Dental Care, we are here to help you protect your smile with modern, personalized, and preventive dental care. If you are experiencing sensitivity, dry mouth, bad breath, enamel wear, mouth ulcers, or gum discomfort, our team can evaluate your oral health and guide you toward the right next steps.
As a trusted dental clinic in Dubai, we combine advanced technology, a comfortable patient experience, and comprehensive dental services to support both oral function and confidence. Whether you need a routine checkup, preventive care, restorative treatment, or a full oral health assessment, our experienced team is ready to help.
Book your appointment with Mint Dental Care today and let us help you maintain a healthier smile from the mouth outward.